- CMS: Medicare Program; Implementation of Prior Authorization for Select Services for the Wasteful and Inappropriate Services Reduction (WISeR) Model
- Public Inspection: CMS: Medicare Program: Implementation of Prior Authorization for Select Services for the Wasteful and Inappropriate Services Reduction Model
- CMS: Secretarial Comments on the CBE's (Battelle Memorial Institute) 2024 Activities: Report to Congress and the Secretary of the Department of Health and Human Services
- HHS: Patient Protection and Affordable Care Act: Marketplace Integrity and Affordability
- HRSA Announces Action to Lower Out-of-Pocket Costs for Life-Saving Medications at Health Centers Nationwide
- Public Inspection: HHS: Patient Protection and Affordable Care Act: Marketplace Integrity and Affordability
- Increased Risk of Cyber Threats Against Healthcare and Public Health Sector
- Eight Hospitals Selected for First Cohort of Rural Hospital Stabilization Program
- Announcing the 2030 Census Disclosure Avoidance Research Program
- CMS: Medicare Program; Hospital Inpatient Prospective Payment Systems for Acute Care Hospitals and the Long-Term Care Hospital Prospective Payment System and Policy Changes and Fiscal Year 2026 Rates; Requirements for Quality Programs; and Other Policy Changes; Correction
- CMS: Medicare Program; Hospital Inpatient Prospective Payment Systems for Acute Care Hospitals and the Long-Term Care Hospital Prospective Payment System and Policy Changes and Fiscal Year 2026 Rates; Requirements for Quality Programs; and Other Policy Changes; Correction
- CMS: Medicare and Medicaid Programs; Contract Year 2026 Policy and Technical Changes to the Medicare Advantage Program, Medicare Prescription Drug Benefit Program, Medicare Cost Plan Program, and Programs of All-Inclusive Care for the Elderly; Correction
- CMS: Medicare and Medicaid Programs; Contract Year 2026 Policy and Technical Changes to the Medicare Advantage Program, Medicare Prescription Drug Benefit Program, Medicare Cost Plan Program, and Programs of All-Inclusive Care for the Elderly; Correction
- CMS: Medicare Program; Prospective Payment System and Consolidated Billing for Skilled Nursing Facilities; Updates to the Quality Reporting Program for Federal Fiscal Year 2026
- CMS: Medicare Program; FY 2026 Hospice Wage Index and Payment Rate Update and Hospice Quality Reporting Program Requirements
Report Highlights Lessons from Dental Utilization During the Pandemic
 The CareQuest Institute for Oral Health released a visual report examining dental procedure utilization during the COVID-19 pandemic, using Medicaid and commercial insurance claims data to find differences in trends by age and insurance type. The authors note a need for the oral health profession to maintain a state of emergency readiness to be able to provide consistent care in the face of future public health emergencies.
The CareQuest Institute for Oral Health released a visual report examining dental procedure utilization during the COVID-19 pandemic, using Medicaid and commercial insurance claims data to find differences in trends by age and insurance type. The authors note a need for the oral health profession to maintain a state of emergency readiness to be able to provide consistent care in the face of future public health emergencies.
Pennsylvania Secretary of Health Highlights Benefits of Community Water Fluoridation During Visit to Shippensburg

Pennsylvania Physician General and Acting Secretary of Health Dr. Denise Johnson was in Shippensburg last week speaking to the safety and benefits of community water fluoridation. In the last few years, Shippensburg faced a fluoridation rollback threat that was overcome with the help of local oral health stakeholders. Dr. Johnson and the Pennsylvania Department of Health are encouraging water systems that do not currently fluoridate to consider initiating for the best interest of their customers. Executive Director Helen Hawkey and Public Health Dental Director Dr. Jonise McDaniel were in attendance.
In Victory for Older Foster Youth, HB 1866 Signed into Law

Pennsylvania Partnerships for Children’s (PPC) priority legislation HB 1866 passed in the last week of the legislative session and was signed into law by Gov. Wolf on November 3rd. Sponsored by Rep. Boback (R-Luzerne), the new law will improve permanency practices for transition age youth in the foster care system. The legislation was introduced in two consecutive legislative sessions, and we are grateful for Rep. Boback’s sponsorship in helping the bill reach the finish line.
Transition age youth are older youth in the foster care system (ages 14 to 21) transitioning to permanency with a caregiver or aging out of the system to adulthood. These young adults often struggle with this life transition. The new law will help foster youth find permanency by:
- Documenting family finding efforts for youth when they are no longer in the system.
- Expanding opportunities for permanency by increasing the age of the goal of Another Planned Permanent Living Arrangement (APPLA) from 16 to 18 years of age.
- Enhancing court accountability regarding suitable transition plans and overseeing services provided to aid in the transition to adulthood.
- Maintaining supportive adult connections to assist transition age youth with building a social safety net when paid professionals are no longer involved.
- Improving data collection to streamline child welfare data from all 67 counties at the state level.
PPC is proud to have helped shepherd HB 1866 through the General Assembly to be signed into law by Gov. Wolf. We will continue to work to improve Pennsylvania’s child welfare system so that foster youth have the opportunity to succeed in life.
Philadelphia Children’s Hospital’s PolicyLab Launches Interactive Platform on Rural Maternal and Child Health

During this year’s National Rural Health Week, PolicyLab will be debuting Our Rural Pennsylvania, an online interactive atlas created by mothers and caregivers to record the everyday places that influence their family’s health. Nearly three years in the making, Our Rural Pennsylvania is the public-facing output of a research project, ‘Understanding the Role of Place in Health and Well-being for families – a Photovoice Project by Moms’. The interdisciplinary project identifies rural-relevant policies and investments to improve maternal and child health in rural communities. Learn more about the project here.
Please join us virtually on November 17 at 5:30pm to celebrate the website launch, hear about the project, and learn about how to use the interactive resource as a resource to advocate for building healthy rural communities. Please RSVP here.
Low-Volume Emergency Departments are More Likely to Use Telehealth for Sepsis Care in a National Rural Telehealth Network
A Research & Policy Brief is available from the Rural Telehealth Research Center:
Sepsis is an expensive disease that is responsible for over 270,000 deaths in the U.S. annually. Early and aggressive treatment with antibiotics and hemodynamic resuscitation have been associated with improved outcomes, but many sepsis patients do not receive guideline-concordant care. Patients treated in low-volume emergency departments (EDs) have 38% higher mortality than those in high-volume EDs suggesting that volume is associated with elements of care that improve survival. Provider-to-provider ED-based telehealth (tele-ED) has been one strategy proposed to improve sepsis care in low-volume EDs. In tele-ED, local ED staff can request consultation with a remote physician and nurse who can connect using a 24-hour on-demand high-definition video connection allowing remote staff to see a patient, review records, provide advice, arrange for inter-hospital transfer, and provide clinical documentation. By connecting a clinician in a high-volume hospital with a care team in a low-volume hospital, rural sepsis patients and providers may benefit from high-volume experience and training even in a local rural facility.
The purpose of this study was to (1) report on the prevalence of tele-ED use for sepsis care across an established network, (2) quantify variation in use between hospitals, and (3) identify predictors of tele-ED consultation in tele-ED-capable hospitals.
USDA Seeks Applications to Support Regional Economic and Community Development Planning to Create Thriving Communities for Rural People

U.S. Department of Agriculture (USDA) Rural Development Under Secretary Xochitl Torres Small announced that USDA is seeking applications to implement regional economic and community development projects to create thriving communities for people in rural America.
The 2018 Farm Bill authorized USDA to make this funding available under the Strategic Economic and Community Development (SECD) initiative to support projects that will help rural people and economies prepare for the future. It can be used to implement projects that are included in multi-jurisdictional and multi-sectoral strategic community investment plans. To learn more, watch USDA’s SECD Initiative video.
HHS Finalizes Physician Payment Rule Strengthening Access to Behavioral Health Services and Whole-Person Care

The U.S. Department of Health and Human Services (HHS), through its Centers for Medicare & Medicaid Services (CMS), is expanding access to behavioral health care, cancer screening coverage, and dental care. The Calendar Year 2023 Physician Fee Schedule (PFS) final rule announced today also promotes innovation and coordinated care in the Medicare program through Accountable Care Organizations (ACOs). This rule directly supports President Biden’s Cancer Moonshot Goal to cut the death rate from cancer by at least 50% and also supports the Administration’s commitment of strengthening behavioral health, which the President outlined in his first State of the Union Address and the comprehensive strategy to tackle the nation’s mental health crisis, which HHS leaders have furthered through the National Tour to Strengthen Mental Health.
“The Biden-Harris Administration is committed to expanding access to vital prevention and treatment services,” said HHS Secretary Xavier Becerra. “Providing whole person support and services through Medicare will improve health and wellbeing for millions of Americans and even save lives.”
“Access to services promoting behavioral health, wellness, and whole-person care is key to helping people achieve the best health possible,” said CMS Administrator Chiquita Brooks-LaSure. “The Physician Fee Schedule final rule ensures that the people we serve will experience coordinated care and that they have access to prevention and treatment services for substance use, mental health services, crisis intervention, and pain care.”
“Together, we are building a stronger Medicare program,” said Deputy Administrator and Director for the Center for Medicare, Dr. Meena Seshamani. “No matter who you are, or what diagnoses you have, these changes will help ensure that Medicare treats the whole person— caring for physical health, behavioral health, and social needs that are integral to health— and ensuring access to the high-quality care all people deserve.”
Coverage for Behavioral Health Services and Opioid Use Disorder Treatment
In line with the 2022 CMS Behavioral Health Strategy, CMS is strengthening access to vital behavioral health services. CMS is making it easier for Medicare beneficiaries to get behavioral health services, by allowing behavioral health clinicians like licensed professional counselors and marriage and family therapists to offer services under general (rather than direct) supervision of the Medicare practitioner. Medicare will pay Opioid Treatment Programs that use telecommunications with patients to initiate treatment with buprenorphine. CMS is also clarifying that Opioid Treatment Programs can bill for opioid use disorder treatment services provided through mobile units, such as vans, in accordance with Substance Abuse and Mental Health Services Administration (SAMHSA) and Drug Enforcement Administration (DEA) guidance. These policies may increase access in rural and other underserved areas.
CMS is also finalizing policies to pay for clinical psychologists and licensed clinical social workers to furnish integrated behavioral health care as part of a primary care team. Finally, Medicare will provide a new monthly payment for comprehensive treatment and management services for patients with chronic pain. These new services offer a whole-person approach to care.
Expanding and Enhancing Accountable Care
CMS is finalizing changes to the Medicare Shared Savings Program, the nation’s largest Accountable Care Organization program, covering more than 11 million people with Medicare and including more than 500,000 health care providers. These policies represent some of the most significant reforms since the program was established in 2011, and the first Accountable Care Organizations (ACOs), which are groups of health care providers who come together to give coordinated, high-quality care to people with Medicare, began participating in 2012. Through these policies, which are central to the Medicare Value-Based Care Strategy, CMS will take important steps toward our 2030 goal of having 100% of Traditional Medicare beneficiaries in an accountable care relationship with their healthcare provider by 2030. CMS is finalizing proposals to incorporate advance shared savings payments to certain new ACOs that can be used to support their participation in the Shared Savings Program, including hiring additional staff or addressing social needs of people with Medicare. CMS is also finalizing a health equity adjustment to an ACO’s quality score, revising the benchmarking methodology, and allowing longer periods of time for ACOs to become accustomed to accountable care before being liable for downside risk, all of which are expected to increase participation in rural and underserved areas.
Reducing Barriers and Expanding Coverage for Colon Cancer Screening
Colon and rectal cancers continue to be a leading cause of death in the United States with even higher new cases and death rates for Black Americans, American Indians, and Alaska Natives. Medicare will now reduce the minimum age for colorectal cancer screening from 50 to 45 years, in alignment with recently revised policy recommendations by the U.S. Preventive Services Task Force. Additionally, Medicare will now cover as a preventive service a follow-on screening colonoscopy after a non-invasive stool-based test returns a positive result, which means that beneficiaries will not have out-of-pocket costs for both tests.
Finalizing Payment for Dental Services that are Integral to Covered Medical Services
CMS is codifying current policies in which Medicare Parts A and B pay for dental services when that service is integral to treating a beneficiary’s medical condition. Medicare will also pay for dental examinations and treatments in more circumstances, such as to eliminate infection preceding an organ transplant and certain cardiac procedures beginning in CY 2023 and prior to treatment for head and neck cancers beginning in CY 2024. Finally, CMS is establishing an annual process to review public input on other circumstances when payment for dental services may be allowed.
Payment Rates for CY 2023
The CY 2023 PFS conversion factor is $33.06, a decrease of $1.55 to the CY 2022 PFS conversion factor of $34.61. This conversion factor reflects the statutorily required update of 0% for CY 2023, expiration of the temporary 3% supplemental increase in PFS payments for CY 2022 provided by the Protecting Medicare and American Farmers From Sequester Cuts Act, and the statutorily required budget neutrality adjustment to account for changes in payment rates.
For a fact sheet on the CY 2023 Physician Fee Schedule Final Rule, please visit: https://www.cms.gov/newsroom/fact-sheets/calendar-year-cy-2023-medicare-physician-fee-schedule-final-rule
For a fact sheet on final changes to the CY 2023 Quality Payment Program, please visit: https://qpp-cm-prod-content.s3.amazonaws.com/uploads/2136/2023%20Quality%20Payment%20Program%20Final%20Rule%20Resources.zip
For a fact sheet on final changes to the Medicare Shared Savings Program, please visit: https://www.cms.gov/newsroom/fact-sheets/calendar-year-cy-2023-medicare-physician-fee-schedule-final-rule-medicare-shared-savings-program
For a CMS blog on behavioral health polices, please visit: https://www.cms.gov/blog/strengthening-behavioral-health-care-people-medicare-0?check_logged_in=1
To view the CY 2023 Physician Fee Schedule and Quality Payment Program final rule, please visit: https://www.cms.gov/files/document/cy2023-physician-fee-schedule-final-rule-cms-1770f.pdf
631 Rural Hospitals at Risk of Closure, by State
Across the U.S., a total of 631 rural hospitals — or about 30 percent of all rural hospitals — are at risk of closing in the immediate or near future due to persistent financial losses on patient services, inadequate revenues to cover expenses, and low financial reserves, according to a report from the Center for Healthcare Quality and Payment Reform.
More than 200 of the rural hospitals in the report are identified as being at immediate risk of closure. These hospitals were losing money on patient services before the COVID-19 pandemic, and they did not have sufficient resources to cover those losses, according to the report. Click here to view the numbers and percentage of rural hospitals by state at risk as of October 2022, based on the Center for Healthcare Quality and Payment Reform analysis.
Rural Adults have Lower Rates of Employer Sponsored Health Insurance in Pennsylvania
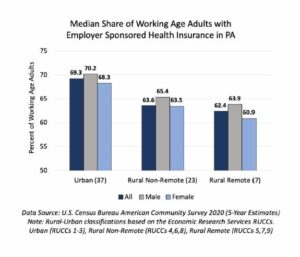 The Penn State Rural Health Disparities Lab in the Department of Biobehavioral Health has released a report showing rates of employer-sponsored health insurance in rural Pennsylvania. Employer sponsored health insurance (ESHI) is typically subsidized by employers, which can reduce the overall cost for employees. Using data from the American Community Survey, we found that working-age adults living in rural areas in Pennsylvania are less likely to have ESHI than those in urban areas. Across all rural-urban categories, females were least likely to have ESHI. The lower rates in rural areas may reflect fewer job opportunities with established ESHI plans. These findings raise concerns about access to the benefits of ESHI in rural contexts, especially for females. Author: Melanie Dececco, RHO Undergraduate Research Assistant
The Penn State Rural Health Disparities Lab in the Department of Biobehavioral Health has released a report showing rates of employer-sponsored health insurance in rural Pennsylvania. Employer sponsored health insurance (ESHI) is typically subsidized by employers, which can reduce the overall cost for employees. Using data from the American Community Survey, we found that working-age adults living in rural areas in Pennsylvania are less likely to have ESHI than those in urban areas. Across all rural-urban categories, females were least likely to have ESHI. The lower rates in rural areas may reflect fewer job opportunities with established ESHI plans. These findings raise concerns about access to the benefits of ESHI in rural contexts, especially for females. Author: Melanie Dececco, RHO Undergraduate Research Assistant
CMS Announces Progress in Promoting Health Equity in Rural Care Access Through Outpatient Hospital and Surgical Center Payment System Final Rule

Critical Access Hospitals and Small Rural Hospitals Can Convert to Rural Emergency Hospitals, Allowing Them to Remain Open to Serve Their Communities
The U.S. Department of Health and Human Services (HHS), through its Centers for Medicare & Medicaid Services (CMS), is improving access to health care — including behavioral health services — in rural communities. CMS is releasing the calendar year (CY) 2023 Hospital Outpatient Prospective Payment System (OPPS) and Ambulatory Surgical Center (ASC) Payment System final rule with comment period. This final rule will allow Critical Access Hospitals (CAHs) and small rural hospitals to convert to a Rural Emergency Hospital (REH), which may be a more sustainable option for rural hospitals facing closure and supports access to care in rural and underserved communities. An REH is a new Medicare provider type that furnishes outpatient services, emergency services, and observation care. In this rule, Medicare will also pay hospital outpatient departments to provide remote behavioral health services to people at home, which will improve access to care in rural communities and promote health equity.
“The Biden-Harris Administration continues to take steps to ensure all Americans, regardless of where they live, have access to high-quality, affordable health care, and this is especially important in rural America, where many hospitals have closed over the past two decades,” said HHS Secretary Xavier Becerra. “By helping rural hospitals stay open, we are helping residents of rural areas get the care they need close to home. Having access to care nearby is not only more convenient, but also leads to better health outcomes — and boosts local economies.”
“CMS is committed to expanding access to care in rural communities and ensuring people with Medicare get the high-quality care they need,” said CMS Administrator Chiquita Brooks-LaSure. “Through the establishment of Rural Emergency Hospitals, supporting clinic visits at rural sole community hospitals and enabling people with Medicare to remotely access behavioral health services in their homes, today’s actions promote patient safety, equity, and quality for these underserved communities. We received broad support for the role Rural Emergency Hospitals can play in advancing health equity and thank stakeholders for their thoughtful input during the public comment period.”
“Establishing Rural Emergency Hospitals can help ensure continued access to critical medical facilities in rural communities,” said Deputy Administrator and Director for the Center for Medicare, Dr. Meena Seshamani. “These facilities are often backbones of communities, but maintaining these businesses and keeping doors open can be challenging. Under today’s final rules regarding this new provider type, we hope to preserve and improve access to care in rural areas and take important steps toward advancing health equity nationwide.”
Updates to OPPS and ASC Payment Rates
CMS is updating the CY 2023 OPPS payment rates and ASC payment rates by 3.8%
Rural Emergency Hospitals
CMS is finalizing conditions of participation, payment rates, and Medicare enrollment requirements for Rural Emergency Hospitals, a new type of Medicare provider that Congress created in the Consolidated Appropriations Act, 2021. These policies for the newly created provider type takes effect on January 1, 2023. Rural hospitals are essential for providing health care in their communities, and the closure of these hospitals limits access to care in areas that are often already underserved. The availability of the REH designation will help support access to health care, particularly emergency services and outpatient services. The REH requirements in this final rule establish a full range of health and safety standards, requirements for services offered, staffing requirements, and physical environment and emergency preparedness standards. REHs will receive additional Medicare payments to help maintain access to a wide array of services in rural areas.
Improving Access to Behavioral Health Services in Rural Areas
CMS is establishing a policy that permits clinical staff of hospital outpatient departments to provide behavioral health services remotely to patients in their homes. CMS first implemented this policy through emergency rulemaking in response to the COVID-19 public health emergency. By making this policy permanent, CMS will ensure access to behavioral health services particularly for rural and other underserved communities, furthering health equity goals.
Enhanced Payment for Non-Opioid Pain Management Drugs and Biologicals
Consistent with the CMS opioid strategy, CMS is finalizing to separately pay for five qualifying non-opioid pain management drugs when administered in ambulatory surgical centers in CY 2023. This ensures that Medicare beneficiaries have access to non-opioid pain management drugs and encourages providers to use non-opioids rather than opioids for pain management.
Payment Adjustments for Additional Costs of Domestic NIOSH-Approved N95 Surgical Respirators
In a future pandemic or increase in community spread of COVID-19, hospitals need to be able to access a reliable supply of NIOSH-approved surgical N95 respirators to protect health care workers and their patients. Sustaining domestic production of these products is important for helping to maintain that reliability. CMS recognizes that hospitals may incur additional costs when purchasing domestically made NIOSH-approved surgical N95 respirators, so this final rule establishes additional hospital payments that would account for these costs.
For a fact sheet on the CY 2023 OPPS/ASC Payment System Final Rule (CMS-1772-FC), please visit: https://www.cms.gov/newsroom/fact-sheets/cy-2023-medicare-hospital-outpatient-prospective-payment-system-and-ambulatory-surgical-center-2
For a fact sheet on Rural Emergency Hospitals, please visit: https://www.cms.gov/newsroom/fact-sheets/cy-2023-medicare-hospital-outpatient-prospective-payment-system-and-ambulatory-surgical-center-1
For a CMS blog on the behavioral health polices in the CY 2023 Physician Fee Schedule and Outpatient Prospective Payment System final rules, please visit: https://www.cms.gov/blog/strengthening-behavioral-health-care-people-medicare-0?check_logged_in=1
The CY 2023 OPPS/ASC Payment System Final Rule can be viewed here: https://www.cms.gov/files/document/cy2023-hospital-outpatient-prospective-payment-system-and-ambulatory-surgical-center-final-rule.pdf
