- VA Announces Expansion of "Close to Me" Cancer Program as Part of the Cancer Moonshot, Bringing Cancer Diagnosis and Treatment Closer to Thousands of Veterans
- Navajo Psychiatrist Bridges Gaps Between Native American Culture and Behavioral Health Care
- Biden-Harris Administration Releases National Strategy for Suicide Prevention and First-Ever Federal Action Plan
- Biden-Harris Administration Takes Historic Action to Increase Access to Quality Care, and Support to Families and Care Workers
- Biden Administration Sets Higher Staffing Mandates. Most Nursing Homes Don't Meet Them.
- Rural Jails Turn to Community Health Workers To Help the Newly Released Succeed
- Rural Communities Face Primary Care Physician Shortage
- Miles for Milk: How Student-Run Grocery Store Reshaped Rural Community's Food Access
- Native Americans Have Shorter Life Spans, and It's Not Just Due to Lack of Health Care
- Promotoras Play Essential Role in Connecting Farmworkers with Health Care in Rural NorCal
- Across the Country, Amish Populations Are on the Rise
- Using Medicaid to Address Young People's Mental Health Needs in School Settings
- Sunsets, Wildlife and Limited Care: Challenges of Aging in Place in Rural America
- City-Country Mortality Gap Widens amid Persistent Holes in Rural Health Care Access
- Tribal Environmental Impact Network
631 Rural Hospitals at Risk of Closure, by State
Across the U.S., a total of 631 rural hospitals — or about 30 percent of all rural hospitals — are at risk of closing in the immediate or near future due to persistent financial losses on patient services, inadequate revenues to cover expenses, and low financial reserves, according to a report from the Center for Healthcare Quality and Payment Reform.
More than 200 of the rural hospitals in the report are identified as being at immediate risk of closure. These hospitals were losing money on patient services before the COVID-19 pandemic, and they did not have sufficient resources to cover those losses, according to the report. Click here to view the numbers and percentage of rural hospitals by state at risk as of October 2022, based on the Center for Healthcare Quality and Payment Reform analysis.
Rural Adults have Lower Rates of Employer Sponsored Health Insurance in Pennsylvania
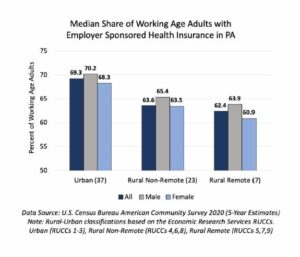 The Penn State Rural Health Disparities Lab in the Department of Biobehavioral Health has released a report showing rates of employer-sponsored health insurance in rural Pennsylvania. Employer sponsored health insurance (ESHI) is typically subsidized by employers, which can reduce the overall cost for employees. Using data from the American Community Survey, we found that working-age adults living in rural areas in Pennsylvania are less likely to have ESHI than those in urban areas. Across all rural-urban categories, females were least likely to have ESHI. The lower rates in rural areas may reflect fewer job opportunities with established ESHI plans. These findings raise concerns about access to the benefits of ESHI in rural contexts, especially for females. Author: Melanie Dececco, RHO Undergraduate Research Assistant
The Penn State Rural Health Disparities Lab in the Department of Biobehavioral Health has released a report showing rates of employer-sponsored health insurance in rural Pennsylvania. Employer sponsored health insurance (ESHI) is typically subsidized by employers, which can reduce the overall cost for employees. Using data from the American Community Survey, we found that working-age adults living in rural areas in Pennsylvania are less likely to have ESHI than those in urban areas. Across all rural-urban categories, females were least likely to have ESHI. The lower rates in rural areas may reflect fewer job opportunities with established ESHI plans. These findings raise concerns about access to the benefits of ESHI in rural contexts, especially for females. Author: Melanie Dececco, RHO Undergraduate Research Assistant
Apply for the HIV & Aging Scholars Program by Nov. 3
Applications are open for the second cohort of the HIV & Aging Scholars Program. This is an interprofessional program open to individuals from any discipline (nursing, social work, pharmacy, medicine, physical therapy, etc.) and people aging with HIV, advocates, peer navigators, case managers, and others from community organizations. Using a cohort-based model, selected candidates will participate in a six-month virtual learning community with national experts and mentors with the goal of improving HIV & aging services in local communities and clinical or community-based settings. Participants will be eligible for CNE and other benefits. View the cohort 1 participants and their projects! Applications for the second cohort are due Nov. 3. Learn more about the program and how to apply.
Pennsylvania Behavioral Health Telehealth Phase II Roadmap is Released
The Office of Mental Health and Substance Abuse Services (OMHSAS) is pleased to share the Pennsylvania Behavioral Health Telehealth Phase II Roadmap, which was developed in collaboration with the OMHSAS Telehealth Steering Committee and Mercer Government Services Consulting. This report focuses on identifying and prioritizing recommendations for short-term and long-term implementation of telehealth services in the Commonwealth. The roadmap includes example documents developed by the Steering Committee that can be used and personalized by the provider when implementing telehealth services. The work of the Steering Committee and other stakeholders has been and will continue to be vital in ensuring that the behavioral health needs of Pennsylvanians continue to be met.
Research Study Shows that Workers are Less Engaged but Still Working Hard
According to a Conference Board survey, 30% of workers say their level of engagement at work—the commitment and connection that employees feel to their work—is lower than six months ago. Lower engagement, however, isn’t necessarily affecting effort: Only 18% say their level of effort has decreased in the last six months. Fifty percent say it’s the same; 31% say it’s increased.
The New Pandemic: Loneliness
Loneliness in America is widespread — and it’s a public health problem. According to a Harvard study, more than one in three Americans are lonely. That rises to 61% when looking at younger people, and 51% among mothers with young kids. Read more.
Nearly 334,000 Providers Left the Healthcare Workforce in 2021
Modern Healthcare reported on Oct. 20, 2022, that nearly 334,000 providers left the healthcare workforce in 2021, driven by burnout and concerns related to the pandemic, according to a report by Definitive Healthcare. About 117,000 were physicians, 53,000 were nurse practitioners, and nearly 23,000 were physician assistants. Read more.
New Report Projects Primary Care Slowing as CVS, Amazon, Walmart Pose Growing Threat
Fierce Healthcare reports that patient demand for primary care and surgical care services remains below pre-pandemic levels, and patient visits “delayed” or “deferred” during the COVID-19 pandemic may be permanently lost, according to a new analysis. At the same time, the number of commercially insured patients decreases while healthcare costs continue to rise. In a 146-page report, Trilliant Health, a healthcare analytics company, outlines 13 macro trends influencing the healthcare industry including population migration, telehealth adoption, competition from new entrants, and healthcare costs. The company’s analysis is based on third-party data resources and the company’s proprietary all-payer claims database that informs longitudinal patient journeys for more than 300 million Americans. Read more.
ACA’s Preventive Care Requirement is Under Attack
Plaintiffs in an Affordable Care Act lawsuit are now asking a federal judge to toss all parts of the law requiring coverage of preventive health services. The filing raises the stakes in the closely watched case, Kelley v. Becerra. If U.S. District Court Judge Reed O’Connor sides with the plaintiffs, millions of Americans could lose coverage for cancer screenings, behavioral counseling, and other recommendations made by the U.S. Preventive Services Task Force. Read more.
Pennsylvania is Rolling Out Online Mental Health Care for K-12
The state of Pennsylvania is piloting digital mental health services in 30 districts for a year, working with the U.K.-based company Kooth to offer access to self-therapy, peer support, and professional support. Read more.
